Neurovascular unit: Difference between revisions
No edit summary Tag: Reverted |
m Open access bot: hdl updated in citation with #oabot. |
||
| (2 intermediate revisions by 2 users not shown) | |||
| Line 46: | Line 46: | ||
=== Alzheimer's disease === |
=== Alzheimer's disease === |
||
[[Alzheimer's disease]] (AD) is the most common type of [[dementia]], a neurodegenerative disease with progressive impairment of behavioral and cognitive functions.<ref>{{cite book | vauthors = Kumar A, Sidhu J, Goyal A, Tsao JW | chapter = Alzheimer Disease |date=2023 | chapter-url = http://www.ncbi.nlm.nih.gov/books/NBK499922/ | title = StatPearls |access-date=2023-06-19 |place=Treasure Island (FL) |publisher=StatPearls Publishing |pmid=29763097 }}</ref> Neuropathologically, there are two major indicators of Alzheimer's: [[neurofibrillary tangle]]s (NFTs) and an accumulation of [[Amyloid beta|amyloid β]] peptide (Aβ) in the brain, known as [[amyloid plaques]], or around blood vessels, known as [[Cerebral amyloid angiopathy|amyloid angiopathy]].<ref>{{cite journal | vauthors = Soto-Rojas LO, Pacheco-Herrero M, Martínez-Gómez PA, Campa-Córdoba BB, Apátiga-Pérez R, Villegas-Rojas MM, Harrington CR, de la Cruz F, Garcés-Ramírez L, Luna-Muñoz J | title = The Neurovascular Unit Dysfunction in Alzheimer's Disease | journal = International Journal of Molecular Sciences | volume = 22 | issue = 4 | pages = 2022 | date = February 2021 | pmid = 33670754 | pmc = 7922832 | doi = 10.3390/ijms22042022 | doi-access = free }}</ref> There is growing support for the vascular hypothesis of AD, which posits that blood vessels are the origin for a variety of pathogenic pathways that lead to neuronal damage and AD.<ref name="Rius-Pérez_2018">{{cite journal | vauthors = Rius-Pérez S, Tormos AM, Pérez S, Taléns-Visconti R | title = Vascular pathology: Cause or effect in Alzheimer disease? | journal = Neurologia | volume = 33 | issue = 2 | pages = 112–120 | date = March 2018 | pmid = 26385017 | doi = 10.1016/j.nrleng.2015.07.008 | doi-access = free }}</ref> Vascular risk factors can result in dysregulation of the neurovascular unit and [[Hypoxia (medical)|hypoxia]]. Destruction of the organization of the blood–brain barrier, decreased cerebral blood flow, and the establishment of an inflammatory context often result in neuronal damage since these factors promote the aggregation of β-amyloid peptide in the brain.<ref name="Rius-Pérez_2018" /> During a review of various consortium data, it was shown that more than 30% of AD cases exhibit [[cerebrovascular disease]] on post-mortem examination, and almost all have evidence of cerebral amyloid angiopathy, microvascular degeneration, and white matter lesions.<ref>{{cite journal | vauthors = Kalaria RN, Ballard C | title = Overlap between pathology of Alzheimer disease and vascular dementia | journal = Alzheimer Disease and Associated Disorders | volume = 13 | issue = Suppl 3 | pages = S115–S123 | date = 1999 | pmid = 10609690 | doi = 10.1097/00002093-199912003-00017 }}</ref> Despite this data, it is still insufficient to reach a pathologic diagnosis, making it unclear whether AD is a cause or a consequence of neuronal dysfunction.<ref name="Iadecola_2004" /><ref name="Rius-Pérez_2018" /> However, considering that AD seems to include a combination of vascular and neurodegenerative processes and that disruption to the vascular physiology occurs early in the disease process, targeting the vascular component may help potentially decelerate the pathologic progression of AD.<ref name="Beishon_2021">{{cite journal | vauthors = Beishon L, Panerai RB | title = The Neurovascular Unit in Dementia: An Opinion on Current Research and Future Directions | journal = Frontiers in Aging Neuroscience | volume = 13 | pages = 721937 | date = 2021 | pmid = 34393765 | pmc = 8355558 | doi = 10.3389/fnagi.2021.721937 | doi-access = free }}</ref> Currently, only a few vascular targets have been the subject of large-scale randomised controlled trials.<ref name="Beishon_2021" /> |
[[Alzheimer's disease]] (AD) is the most common type of [[dementia]], a neurodegenerative disease with progressive impairment of behavioral and cognitive functions.<ref>{{cite book | vauthors = Kumar A, Sidhu J, Goyal A, Tsao JW | chapter = Alzheimer Disease |date=2023 | chapter-url = http://www.ncbi.nlm.nih.gov/books/NBK499922/ | title = StatPearls |access-date=2023-06-19 |place=Treasure Island (FL) |publisher=StatPearls Publishing |pmid=29763097 }}</ref> Neuropathologically, there are two major indicators of Alzheimer's: [[neurofibrillary tangle]]s (NFTs) and an accumulation of [[Amyloid beta|amyloid β]] peptide (Aβ) in the brain, known as [[amyloid plaques]], or around blood vessels, known as [[Cerebral amyloid angiopathy|amyloid angiopathy]].<ref>{{cite journal | vauthors = Soto-Rojas LO, Pacheco-Herrero M, Martínez-Gómez PA, Campa-Córdoba BB, Apátiga-Pérez R, Villegas-Rojas MM, Harrington CR, de la Cruz F, Garcés-Ramírez L, Luna-Muñoz J | title = The Neurovascular Unit Dysfunction in Alzheimer's Disease | journal = International Journal of Molecular Sciences | volume = 22 | issue = 4 | pages = 2022 | date = February 2021 | pmid = 33670754 | pmc = 7922832 | doi = 10.3390/ijms22042022 | doi-access = free }}</ref> There is growing support for the vascular hypothesis of AD, which posits that blood vessels are the origin for a variety of pathogenic pathways that lead to neuronal damage and AD.<ref name="Rius-Pérez_2018">{{cite journal | vauthors = Rius-Pérez S, Tormos AM, Pérez S, Taléns-Visconti R | title = Vascular pathology: Cause or effect in Alzheimer disease? | journal = Neurologia | volume = 33 | issue = 2 | pages = 112–120 | date = March 2018 | pmid = 26385017 | doi = 10.1016/j.nrleng.2015.07.008 | doi-access = free | hdl = 10550/92379 | hdl-access = free }}</ref> Vascular risk factors can result in dysregulation of the neurovascular unit and [[Hypoxia (medical)|hypoxia]]. Destruction of the organization of the blood–brain barrier, decreased cerebral blood flow, and the establishment of an inflammatory context often result in neuronal damage since these factors promote the aggregation of β-amyloid peptide in the brain.<ref name="Rius-Pérez_2018" /> During a review of various consortium data, it was shown that more than 30% of AD cases exhibit [[cerebrovascular disease]] on post-mortem examination, and almost all have evidence of cerebral amyloid angiopathy, microvascular degeneration, and white matter lesions.<ref>{{cite journal | vauthors = Kalaria RN, Ballard C | title = Overlap between pathology of Alzheimer disease and vascular dementia | journal = Alzheimer Disease and Associated Disorders | volume = 13 | issue = Suppl 3 | pages = S115–S123 | date = 1999 | pmid = 10609690 | doi = 10.1097/00002093-199912003-00017 }}</ref> Despite this data, it is still insufficient to reach a pathologic diagnosis, making it unclear whether AD is a cause or a consequence of neuronal dysfunction.<ref name="Iadecola_2004" /><ref name="Rius-Pérez_2018" /> However, considering that AD seems to include a combination of vascular and neurodegenerative processes and that disruption to the vascular physiology occurs early in the disease process, targeting the vascular component may help potentially decelerate the pathologic progression of AD.<ref name="Beishon_2021">{{cite journal | vauthors = Beishon L, Panerai RB | title = The Neurovascular Unit in Dementia: An Opinion on Current Research and Future Directions | journal = Frontiers in Aging Neuroscience | volume = 13 | pages = 721937 | date = 2021 | pmid = 34393765 | pmc = 8355558 | doi = 10.3389/fnagi.2021.721937 | doi-access = free }}</ref> Currently, only a few vascular targets have been the subject of large-scale randomised controlled trials.<ref name="Beishon_2021" /> |
||
=== Huntington's disease === |
=== Huntington's disease === |
||
| Line 54: | Line 54: | ||
{{Reflist}} |
{{Reflist}} |
||
[[Category: |
[[Category:Neurology]] |
||
Latest revision as of 05:26, 16 December 2024
The neurovascular unit (NVU) comprises the components of the brain that collectively regulate cerebral blood flow in order to deliver the requisite nutrients to activated neurons.[1] The NVU addresses the brain's unique dilemma of having high energy demands yet low energy storage capacity. In order to function properly, the brain must receive substrates for energy metabolism–mainly glucose–in specific areas, quantities, and times.[2] Neurons do not have the same ability as, for example, muscle cells, which can use up their energy reserves and refill them later; therefore, cerebral metabolism must be driven in the moment. The neurovascular unit facilitates this ad hoc delivery and, thus, ensures that neuronal activity can continue seamlessly.[2]
The neurovascular unit was formalized as a concept in 2001, at the inaugural Stroke Progress Review Group of the National Institute of Neurological Disorders and Stroke (NINDS).[1] In prior years, the importance of both neurons and cerebral vasculature was well known; however, their interconnected relationship was not. The two were long considered distinct entities which, for the most part, operated independently. Since 2001, though, the rapid increase of scientific papers citing the neurovascular unit represents the growing understanding of the interactions that occur between the brain’s cells and blood vessels.[1]
The neurovascular unit consists of neurons, astrocytes, vasculature (endothelial and vascular mural cells), the vasomotor apparatus (smooth muscle cells and pericytes), and microglia.[1] Together these function in the homeostatic haemodynamic response of cerebral hyperaemia.[3] Cerebral hyperaemia is a fundamental central nervous system mechanism of homeostasis that increases blood supply to neural tissue when necessary.[3] This mechanism controls oxygen and nutrient levels using vasodilation and vasoconstriction in a multidimensional process involving the many cells of the neurovascular unit, along with multiple signaling molecules.[1] The interactions between the components of the NVU allow it to sense neurons' needs of oxygen and glucose and, in turn, trigger the appropriate vasodilatory or vasoconstrictive responses.[3] Neuronal activity[4] as well as astrocytes[5] can therefore participate in CNV, both by inducing vasodilation and vasoconstriction[6].Thus, the NVU provides the architecture behind neurovascular coupling, which connects neuronal activity to cerebral blood flow and highlights the interdependence of their development, structure, and function.[1]
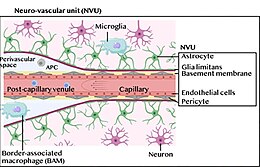
The temporal and spatial link between cerebral blood flow and neuronal activity allows the former to serve as a proxy for the latter. Neuroimaging techniques that directly or indirectly monitor blood flow, such as fMRI and PET scans, can, thus, measure and locate activity in the brain with precision.[1] Imaging of the brain also allows researchers to better understand the neurovascular unit and its many complexities. Furthermore, any impediments to the function of the neurovascular system will prevent neurons from receiving the appropriate nutrients. A complete stoppage for only a few minutes, which could be caused by arterial occlusion or heart failure, can result in permanent damage and death. Dysfunction in the NVU is also associated with neurodegenerative diseases including Alzheimer's and Huntington's disease.[1]
Function
[edit]Anatomical components
[edit]The neurovascular unit is made up of vascular cells (including endothelium, pericytes, and smooth muscle cells), glia (astrocytes and microglia), and neurons with synaptic junctions for signaling.[1] Cerebral vessels, namely arterioles and the perivascular compartment, form the network of the NVU.[7] Arterioles are made up of pial vessels and arterioles, and the perivascular compartment includes perivascular macrophages in addition to Mato, pial, and mast cells. Cerebral blood flow is a critical component of this overall system and it is facilitated by the neck arteries. Segmented vascular resistance, or the amount of flow control that each section of the brain maintains, is measured as the ratio of the blood pressure gradient to blood flow volume.[8] The blood flow within the NVU is a low resistance channel that allows blood to be distributed to different parts of the body.[9] The cells of the NVU sense the needs of neural tissue and release many different mediators that engage in signaling pathways and initiate effector systems such as the myogenic effect; these mediators trigger the vascular smooth muscle cells to increase blood flow through vasodilation or to reduce blood flow by vasoconstriction.[3][1][10] This is recognized as a multidimensional response that operates across the cerebrovascular network as a whole.[1]
Blood–brain barrier
[edit]The cells of the neurovascular unit also make up the blood–brain barrier (BBB), which plays an important role in maintaining the microenvironment of the brain.[11] In addition to regulating the exit and entrance of blood, the blood–brain barrier also filters toxins that may cause inflammation, injury, and disease.[12] The overall microvasculature unit functions as a defense for the central nervous system.[11] Encompassed within the BBB are two types of blood vessels: endothelial and mural cells. Endothelial cells form the wall of the BBB, while mural cells exist on the outer surface of this layer of endothelial cells. The mural cells also have their own abluminal layer which hosts pericytes that work to maintain the permeability of the barrier, and the epithelial cells filter the amount of toxins entering. These cells connect to different segments of the vascular tree that exist within the brain.[12]
Neurovascular coupling
[edit]Cellular processes critically rely on the production of adenosine triphosphate (ATP), which requires glucose and oxygen.[13] These need to be delivered to areas in the brain with consistency via cerebral blood flow. In order for the brain to receive enough blood flow when in high demand, coupling occurs between neurons and CBF. Neurovascular coupling encompasses the changes in cerebral blood flow that occur in response to the level of neuronal activity.[1][14][15] When the brain needs to exert more energy, there is an associated increase in the level of blood flow to compensate for this. The brain does not have a place where it stores energy, and, therefore, the response of blood flow has to be immediate so that crucial functions for continued life can persist. Difficulties arise when angiotensin proteins are present in higher concentrations, as there is an associated increase in blood flow that leads to hypertension and potential disorders.[8] Furthermore, modern imaging techniques have allowed researchers to view and study cerebral blood flow in a noninvasive manner. However, imaging deep brain structures in vivo is challenging. Therefore, NVC can be studied on ex vivo brain slices maintained in survival conditions.[16][17] Ultimately, neurovascular coupling promotes brain health by moderating proper cerebral blood flow. There is still much more to be discovered about it, though; and, due to the difficulty of in vivo research, the growing body of knowledge on neurovascular coupling relies heavily on ex vivo techniques for imaging the neurovascular unit.
Imaging
[edit]The neurovascular unit enables imaging techniques to measure neuronal activity by tracking blood flow. Various other types of neuroimaging also allow the NVU itself to be studied by providing visual insights into the complex interactions between neurons, glial cells, and blood vessels in the brain.
Fluorescence microscopy
[edit]Fluorescence microscopy is a widely used imaging technique that utilizes fluorescent probes to visualize specific molecules or structures within the neurovascular unit.[18] It allows researchers to label and track cellular components, such as neurons, astrocytes, and blood vessel markers, with high specificity.[19] Fluorescence imaging offers excellent spatial resolution, allowing for detailed visualization of cellular morphology and localized molecular interactions.[20] By using different fluorophores, researchers can simultaneously examine multiple cellular components and molecular pathways of the neurovascular unit. However, limited tissue penetration depth, photobleaching, and phototoxicity negatively impact the potential for long-term imaging studies.[20]
Electron microscopy
[edit]Electron microscopy provides details of the neurovascular unit at the nanometer scale by using a focused beam of electrons instead of light, enabling higher resolution imaging. Transmission electron microscopy images thin tissue sections, providing detailed information about the fine cellular structures, including synapses and organelles.[21] Scanning electron microscopy, on the other hand, provides 3D information by scanning a focused electron beam across the sample's surface, allowing for the visualization of the topography of neurovascular unit components.[22] Electron microscopy techniques are, thus, invaluable for studying the precise cellular and subcellular interactions within the NVU.[23] However, it requires sample preparation involving fixation, dehydration, and staining, which can introduce artifacts, and it is not suitable for live or large-scale imaging due to its time-consuming nature.
Magnetic resonance imaging
[edit]Magnetic resonance imaging (MRI) is a non-invasive imaging technique that uses strong magnetic fields and radio waves to generate detailed images of the brain's anatomy and function.[24] It can provide information about blood flow, oxygenation levels, and structural characteristics of the neurovascular unit. The functional MRI (fMRI) allows researchers to study brain activity by measuring changes in blood oxygenation associated with neural activity, thus classifying it as a blood-oxygen-level-dependent imaging (BOLD imaging) technique. Diffusion MRI (dMRI) provides insights into the brain's structural connectivity by tracking the diffusion of water molecules in its tissue.[25] MRI, in general, has excellent spatial resolution and can be used for both human and animal studies, making it a valuable tool for studying the neurovascular unit in vivo. It has limited temporal resolution, though, and its ability to visualize finer cellular and molecular details within the neurovascular unit is relatively lower compared to microscopy techniques.
Optical coherence tomography
[edit]Optical coherence tomography (OCT) is an imaging technique that utilizes low-coherence interferometry to generate high-resolution cross-sectional images of biological tissues.[26] It can, thus, provide information about the microstructure and vascular network of the neurovascular unit.[27] More specifically, OCT has been used to study cerebral blood flow dynamics, changes in vessel diameter, and blood–brain barrier integrity. It also has real-time imaging capabilities and can, thus, be effectively applied in both clinical and preclinical settings.[27] Downsides of optical coherence tomography include limited depth penetration in highly scattering tissues and a lower resolution in increasing depth, which can limit its application in deep brain regions.[26]
Clinical significance
[edit]Neurovascular failure
[edit]Neurovascular failure, or neurovascular disease, refers to a range of conditions that negatively affect the function of blood vessels in the brain and spinal cord.[28] While the exact mechanisms behind neurovascular disease are unknown, people with inherited conditions (such as a family history of heart disease, diabetes, and/or high cholesterol), poor lifestyle choices, genetic changes during pregnancy, physical trauma, and other specific genetic characteristics are generally at higher risk.[28] In particular, neurovascular failure can be caused by problems arising in the blood vessels, including blockages (embolism), clot formation (thrombosis), narrowing (stenosis), and rupture (hemorrhage). In response to pathogenic stimuli, such as tissue hypoxia, signaling pathways involved in neurovascular coupling are impaired.[29][30] Neuronal injury is often preceded by the expression and release of pro-angiogenic factors, such as vascular endothelial growth factor (VEGF); in addition to this, the upregulation of astrocyte receptors in endothelial cells can stimulate endothelial proliferation and migration, which can dangerously increase blood–brain barrier (BBB) permeability.[29] Ultimately, vascular dysfunction results in decreased cerebral blood flow and abnormalities in the blood–brain barrier, which poses a threat to the normal functioning of the brain.[31]
Effects of neurovascular failure
[edit]Efficient blood supply to the brain is extremely significant to its normal functioning, and improper blood flow can lead to potentially devastating neurological consequences.[31] Alterations of vascular regulatory mechanisms lead to brain dysfunction and disease. The emerging view is that neurovascular dysfunction is a feature not only of cerebrovascular pathologies, such as stroke, but also of neurodegenerative conditions, such as Alzheimer's disease.[32] While studies are still ongoing to determine the precise effects of neurovascular failure, there is emerging evidence that neurovascular dysfunction plays a pivotal role in the degeneration of the nervous system, which contrasts the typical view that neurodegeneration is caused by intrinsic neuronal effects.[29][33] The breakdown of neurovascular coupling (e.g., modulations in neuronal activity that cause changes in local blood flow[8]) and the pathophysiology of the NVU is commonly observed across a wide variety of neurological and psychiatric disorders, including Alzheimer’s disease.[29] The combination of recent hypotheses and evidence suggests that the pathophysiology of the NVU may contribute to cognitive impairment and be an initiating trigger for neurological manifestations of diseases such as Alzheimer's and dementia.[34][30] Ultimately, despite the vast amount of current literature supporting vascular contributions to neurological phenotypes, there is still much to be investigated, especially with respect to the effect of neurovasculature on neurological diseases; namely, whether the initiating event occurs at the neuronal level and "mobilizes" vascular response or the vascular event triggers neuronal dysfunction.[29][30]
Alzheimer's disease
[edit]Alzheimer's disease (AD) is the most common type of dementia, a neurodegenerative disease with progressive impairment of behavioral and cognitive functions.[35] Neuropathologically, there are two major indicators of Alzheimer's: neurofibrillary tangles (NFTs) and an accumulation of amyloid β peptide (Aβ) in the brain, known as amyloid plaques, or around blood vessels, known as amyloid angiopathy.[36] There is growing support for the vascular hypothesis of AD, which posits that blood vessels are the origin for a variety of pathogenic pathways that lead to neuronal damage and AD.[37] Vascular risk factors can result in dysregulation of the neurovascular unit and hypoxia. Destruction of the organization of the blood–brain barrier, decreased cerebral blood flow, and the establishment of an inflammatory context often result in neuronal damage since these factors promote the aggregation of β-amyloid peptide in the brain.[37] During a review of various consortium data, it was shown that more than 30% of AD cases exhibit cerebrovascular disease on post-mortem examination, and almost all have evidence of cerebral amyloid angiopathy, microvascular degeneration, and white matter lesions.[38] Despite this data, it is still insufficient to reach a pathologic diagnosis, making it unclear whether AD is a cause or a consequence of neuronal dysfunction.[32][37] However, considering that AD seems to include a combination of vascular and neurodegenerative processes and that disruption to the vascular physiology occurs early in the disease process, targeting the vascular component may help potentially decelerate the pathologic progression of AD.[39] Currently, only a few vascular targets have been the subject of large-scale randomised controlled trials.[39]
Huntington's disease
[edit]Huntington's disease (HD) is an autosomal dominant neurodegenerative disease caused by an abnormal repetition of the CAG trinucleotide repeat within the Huntingtin gene (Htt).[40] Common features of Huntington's include involuntary movements (chorea), bradykinesia, psychiatric symptoms, and cognitive decline, all of which are accelerated through neuronal cell death.[41][42] The idea that neurovascular impairments may contribute to early neuronal cell loss in Huntington’s disease has been attracting significant attention in the HD community. Reduced cerebral blood flow, increased small vessel density, and increased blood–brain barrier (BBB) permeability–all traits of neurovascular dysfunction–have been reported in both rodent and patient post-mortem tissue.[43][44][45] Preliminary findings support that neurovascular alterations occur in Huntington's disease and may contribute to its early neuropathology.[46] It has also been proposed that neurovascular dysregulation manifests earlier in Huntington's than other pathologies, triggering innate immune signaling and a reduction of protein levels critical for maintaining the blood–brain barrier.[47] While neurovascular failure in HD pathogenesis is still being tested, recent work supports clinical application. For example, immunohistological assays revealed vessel aberrations in brain tissue, establishing the early onset of such aberrations as a potential biomarker for early Huntington's diagnosis.[33]
References
[edit]- ^ a b c d e f g h i j k l Iadecola C (September 2017). "The Neurovascular Unit Coming of Age: A Journey through Neurovascular Coupling in Health and Disease". Neuron. 96 (1): 17–42. doi:10.1016/j.neuron.2017.07.030. PMC 5657612. PMID 28957666.
- ^ a b Stackhouse TL, Mishra A (2021-07-12). "Neurovascular Coupling in Development and Disease: Focus on Astrocytes". Frontiers in Cell and Developmental Biology. 9: 702832. doi:10.3389/fcell.2021.702832. PMC 8313501. PMID 34327206.
- ^ a b c d Muoio V, Persson PB, Sendeski MM (April 2014). "The neurovascular unit - concept review". Acta Physiologica. 210 (4): 790–798. doi:10.1111/apha.12250. PMID 24629161. S2CID 25274791.
- ^ Cauli B, Tong XK, Rancillac A, Serluca N, Lambolez B, Rossier J, et al. (October 2004). "Cortical GABA interneurons in neurovascular coupling: relays for subcortical vasoactive pathways". The Journal of Neuroscience. 24 (41): 8940–8949. doi:10.1523/JNEUROSCI.3065-04.2004. PMC 6730057. PMID 15483113.
The expression of vasoactive intestinal peptide (VIP) or nitric oxide synthase (NOS) in interneurons induces dilation, while somatostatin (SOM) induces contraction. Direct perfusion of VIP and NO donors onto the slices caused microvessel dilation, whereas neuropeptide Y (NPY) and SOM induced vasoconstriction. Vasomotor interneurons established contacts with local microvessels and received somatic and dendritic afferents from acetylcholine (ACh) and serotonin (5-HT) pathways, varying by interneuron subtype. Our results demonstrate the capability of specific subsets of cortical GABA interneurons to transmute neuronal signals into vascular responses and suggest that they could serve as local integrators of neurovascular coupling for subcortical vasoactive pathways.
- ^ Carmignoto G, Gómez-Gonzalo M (May 2010). "The contribution of astrocyte signalling to neurovascular coupling". Brain Research Reviews. 63 (1–2): 138–148. doi:10.1016/j.brainresrev.2009.11.007. PMID 19948187.
- ^ Rancillac A, Rossier J, Guille M, Tong XK, Geoffroy H, Amatore C, et al. (June 2006). "Glutamatergic Control of Microvascular Tone by Distinct GABA Neurons in the Cerebellum". The Journal of Neuroscience. 26 (26): 6997–7006. doi:10.1523/JNEUROSCI.5515-05.2006. PMC 6673912. PMID 16807329.
Cerebellar stellate and Purkinje cells play distinct roles in neurovascular coupling by dilating and constricting neighboring microvessels, respectively. This highlights the specialized functions of different neuron types in regulating cerebral blood flow.
- ^ Filosa JA (2010). "Vascular tone and neurovascular coupling: considerations toward an improved in vitro model". Frontiers in Neuroenergetics. 2. doi:10.3389/fnene.2010.00016. PMC 2928708. PMID 20802803.
- ^ a b c Phillips AA, Chan FH, Zheng MM, Krassioukov AV, Ainslie PN (April 2016). "Neurovascular coupling in humans: Physiology, methodological advances and clinical implications". Journal of Cerebral Blood Flow and Metabolism. 36 (4): 647–664. doi:10.1177/0271678X15617954. PMC 4821024. PMID 26661243.
- ^ Cipolla MJ (2009). "Chapter 5, Control of Cerebral Blood Flow". The Cerebral Circulation. San Rafael (CA): Morgan & Claypool Life Sciences.
- ^ Rancillac A, Rossier J, Guille M, Tong XK, Geoffroy H, Amatore C, et al. (June 2006). "Glutamatergic Control of Microvascular Tone by Distinct GABA Neurons in the Cerebellum". The Journal of Neuroscience. 26 (26): 6997–7006. doi:10.1523/JNEUROSCI.5515-05.2006. PMC 6673912. PMID 16807329.
- ^ a b Ahmad A, Patel V, Xiao J, Khan MM (November 2020). "The Role of Neurovascular System in Neurodegenerative Diseases". Molecular Neurobiology. 57 (11): 4373–4393. doi:10.1007/s12035-020-02023-z. PMID 32725516. S2CID 220843844.
- ^ a b Daneman R, Prat A (January 2015). "The blood-brain barrier". Cold Spring Harbor Perspectives in Biology. 7 (1): a020412. doi:10.1101/cshperspect.a020412. PMC 4292164. PMID 25561720.
- ^ Pasley BN, Freeman RD (2008-03-11). "Neurovascular coupling". Scholarpedia. 3 (3): 5340. Bibcode:2008SchpJ...3.5340P. doi:10.4249/scholarpedia.5340. ISSN 1941-6016.
- ^ Rancillac A, Rossier J, Guille M, Tong XK, Geoffroy H, Amatore C, et al. (June 2006). "Glutamatergic Control of Microvascular Tone by Distinct GABA Neurons in the Cerebellum". The Journal of Neuroscience. 26 (26): 6997–7006. doi:10.1523/JNEUROSCI.5515-05.2006. PMC 6673912. PMID 16807329.
- ^ Cauli B, Tong XK, Rancillac A, Serluca N, Lambolez B, Rossier J, et al. (October 2004). "Cortical GABA interneurons in neurovascular coupling: relays for subcortical vasoactive pathways". The Journal of Neuroscience. 24 (41): 8940–8949. doi:10.1523/JNEUROSCI.3065-04.2004. PMC 6730057. PMID 15483113.
- ^ Scharbarg E, Daenens M, Lemaître F, Geoffroy H, Guille-Collignon M, Gallopin T, et al. (January 2016). "Astrocyte-derived adenosine is central to the hypnogenic effect of glucose". Scientific Reports. 6 (1): 19107. Bibcode:2016NatSR...619107S. doi:10.1038/srep19107. PMC 4709579. PMID 26755200.
Using infrared videomicroscopy on ex vivo brain slices, we established that glucose induces vasodilation specifically in the Ventrolateral Preoptic Nucleus (VLPO) via astrocytic release of adenosine.
- ^ Scharbarg E, Walter A, Lecoin L, Gallopin T, Lemaître F, Guille-Collignon M, et al. (March 2023). "Prostaglandin D2 Controls Local Blood Flow and Sleep-Promoting Neurons in the VLPO via Astrocyte-Derived Adenosine" (PDF). ACS Chemical Neuroscience. 14 (6): 1063–1070. doi:10.1021/acschemneuro.2c00660. PMID 36847485.
Measurements of vasodilatory responses and electrophysiological recordings reveal that, in response to PGD2 application, adenosine release induces A2A receptor (A2AR)-mediated dilation of blood vessels and activation of Ventrolateral Preoptic Nucleus (VLPO) sleep-promoting neurons. Collectively, our results elucidate the PGD2 signaling pathway in the VLPO, demonstrating its role in controlling local blood flow and activating sleep-promoting neurons via astrocyte-derived adenosine.
- ^ Chen S, Wang Z, Zhang D, Wang A, Chen L, Cheng H, et al. (October 2020). "Miniature Fluorescence Microscopy for Imaging Brain Activity in Freely-Behaving Animals". Neuroscience Bulletin. 36 (10): 1182–1190. doi:10.1007/s12264-020-00561-z. PMC 7532237. PMID 32797396.
- ^ Mai-Morente SP, Marset VM, Blanco F, Isasi EE, Abudara V (May 2021). "A nuclear fluorescent dye identifies pericytes at the neurovascular unit". Journal of Neurochemistry. 157 (4): 1377–1391. doi:10.1111/jnc.15193. hdl:20.500.12008/26846. PMID 32974913.
- ^ a b Sanderson MJ, Smith I, Parker I, Bootman MD (October 2014). "Fluorescence microscopy". Cold Spring Harbor Protocols. 2014 (10): pdb.top071795. doi:10.1101/pdb.top071795. PMC 4711767. PMID 25275114.
- ^ Nahirney PC, Tremblay ME (2021). "Brain Ultrastructure: Putting the Pieces Together". Frontiers in Cell and Developmental Biology. 9: 629503. doi:10.3389/fcell.2021.629503. PMC 7930431. PMID 33681208.
- ^ Knott G, Marchman H, Wall D, Lich B (March 2008). "Serial section scanning electron microscopy of adult brain tissue using focused ion beam milling". The Journal of Neuroscience. 28 (12): 2959–2964. doi:10.1523/JNEUROSCI.3189-07.2008. PMC 6670719. PMID 18353998.
- ^ Kubota Y, Sohn J, Kawaguchi Y (2018). "Large Volume Electron Microscopy and Neural Microcircuit Analysis". Frontiers in Neural Circuits. 12: 98. doi:10.3389/fncir.2018.00098. PMC 6240581. PMID 30483066.
- ^ "Magnetic Resonance Imaging (MRI)". National Institute of Biomedical Imaging and Bioengineering. Retrieved 2023-06-19.
- ^ Mueller BA, Lim KO, Hemmy L, Camchong J (September 2015). "Diffusion MRI and its Role in Neuropsychology". Neuropsychology Review. 25 (3): 250–271. doi:10.1007/s11065-015-9291-z. PMC 4807614. PMID 26255305.
- ^ a b Fujimoto JG, Pitris C, Boppart SA, Brezinski ME (2000-01-01). "Optical coherence tomography: an emerging technology for biomedical imaging and optical biopsy". Neoplasia. 2 (1–2): 9–25. doi:10.1038/sj.neo.7900071. PMC 1531864. PMID 10933065.
- ^ a b Anagnostakou V, Ughi GJ, Puri AS, Gounis MJ (October 2021). "Optical Coherence Tomography for Neurovascular Disorders". Neuroscience. Brain imaging. 474: 134–144. doi:10.1016/j.neuroscience.2021.06.008. PMID 34126186.
- ^ a b "Cerebrovascular Disease". Penn Medicine. Philadelphia, PA: University of Pennsylvania. Retrieved 2023-06-19.
- ^ a b c d e Stanimirovic DB, Friedman A (July 2012). "Pathophysiology of the neurovascular unit: disease cause or consequence?". Journal of Cerebral Blood Flow and Metabolism. 32 (7): 1207–1221. doi:10.1038/jcbfm.2012.25. PMC 3390807. PMID 22395208.
- ^ a b c Shabir O, Berwick J, Francis SE (October 2018). "Neurovascular dysfunction in vascular dementia, Alzheimer's and atherosclerosis". BMC Neuroscience. 19 (1): 62. doi:10.1186/s12868-018-0465-5. PMC 6192291. PMID 30333009.
- ^ a b Nelson AR, Sweeney MD, Sagare AP, Zlokovic BV (May 2016). "Neurovascular dysfunction and neurodegeneration in dementia and Alzheimer's disease". Biochimica et Biophysica Acta (BBA) - Molecular Basis of Disease. Vascular contributions to cognitive impairment and dementia (VCID). 1862 (5): 887–900. doi:10.1016/j.bbadis.2015.12.016. PMC 4821735. PMID 26705676.
- ^ a b Iadecola C (May 2004). "Neurovascular regulation in the normal brain and in Alzheimer's disease". Nature Reviews. Neuroscience. 5 (5): 347–360. doi:10.1038/nrn1387. PMID 15100718. S2CID 36555564.
- ^ a b Lin CY, Hsu YH, Lin MH, Yang TH, Chen HM, Chen YC, et al. (December 2013). "Neurovascular abnormalities in humans and mice with Huntington's disease". Experimental Neurology. 250: 20–30. doi:10.1016/j.expneurol.2013.08.019. PMID 24036415. S2CID 9613243.
- ^ Kapasi A, Schneider JA (May 2016). "Vascular contributions to cognitive impairment, clinical Alzheimer's disease, and dementia in older persons". Biochimica et Biophysica Acta (BBA) - Molecular Basis of Disease. 1862 (5): 878–886. doi:10.1016/j.bbadis.2015.12.023. PMC 11062590. PMID 26769363.
- ^ Kumar A, Sidhu J, Goyal A, Tsao JW (2023). "Alzheimer Disease". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 29763097. Retrieved 2023-06-19.
- ^ Soto-Rojas LO, Pacheco-Herrero M, Martínez-Gómez PA, Campa-Córdoba BB, Apátiga-Pérez R, Villegas-Rojas MM, et al. (February 2021). "The Neurovascular Unit Dysfunction in Alzheimer's Disease". International Journal of Molecular Sciences. 22 (4): 2022. doi:10.3390/ijms22042022. PMC 7922832. PMID 33670754.
- ^ a b c Rius-Pérez S, Tormos AM, Pérez S, Taléns-Visconti R (March 2018). "Vascular pathology: Cause or effect in Alzheimer disease?". Neurologia. 33 (2): 112–120. doi:10.1016/j.nrleng.2015.07.008. hdl:10550/92379. PMID 26385017.
- ^ Kalaria RN, Ballard C (1999). "Overlap between pathology of Alzheimer disease and vascular dementia". Alzheimer Disease and Associated Disorders. 13 (Suppl 3): S115–S123. doi:10.1097/00002093-199912003-00017. PMID 10609690.
- ^ a b Beishon L, Panerai RB (2021). "The Neurovascular Unit in Dementia: An Opinion on Current Research and Future Directions". Frontiers in Aging Neuroscience. 13: 721937. doi:10.3389/fnagi.2021.721937. PMC 8355558. PMID 34393765.
- ^ Nopoulos PC (March 2016). "Huntington disease: a single-gene degenerative disorder of the striatum". Dialogues in Clinical Neuroscience. 18 (1): 91–98. doi:10.31887/DCNS.2016.18.1/pnopoulos. PMC 4826775. PMID 27069383.
- ^ Novak MJ, Tabrizi SJ (June 2010). "Huntington's disease". BMJ. 340: c3109. doi:10.1136/bmj.c3109. PMID 20591965. S2CID 16061768.
- ^ Jakel RJ, Maragos WF (June 2000). "Neuronal cell death in Huntington's disease: a potential role for dopamine". Trends in Neurosciences. 23 (6): 239–245. doi:10.1016/s0166-2236(00)01568-x. PMID 10838590. S2CID 25754639.
- ^ Chen JJ, Salat DH, Rosas HD (January 2012). "Complex relationships between cerebral blood flow and brain atrophy in early Huntington's disease". NeuroImage. 59 (2): 1043–1051. doi:10.1016/j.neuroimage.2011.08.112. PMC 3787075. PMID 21945790.
- ^ Hsiao HY, Chen YC, Huang CH, Chen CC, Hsu YH, Chen HM, et al. (August 2015). "Aberrant astrocytes impair vascular reactivity in Huntington disease". Annals of Neurology. 78 (2): 178–192. doi:10.1002/ana.24428. PMID 25914140. S2CID 30714012.
- ^ Drouin-Ouellet J, Sawiak SJ, Cisbani G, Lagacé M, Kuan WL, Saint-Pierre M, et al. (August 2015). "Cerebrovascular and blood-brain barrier impairments in Huntington's disease: Potential implications for its pathophysiology". Annals of Neurology. 78 (2): 160–177. doi:10.1002/ana.24406. PMID 25866151. S2CID 15993646.
- ^ Chan ST, Mercaldo ND, Kwong KK, Hersch SM, Rosas HD (2021). "Impaired Cerebrovascular Reactivity in Huntington's Disease". Frontiers in Physiology. 12: 663898. doi:10.3389/fphys.2021.663898. PMC 8334185. PMID 34366879.
- ^ Garcia FJ, Sun N, Lee H, Godlewski B, Mathys H, Galani K, et al. (March 2022). "Single-cell dissection of the human brain vasculature". Nature. 603 (7903): 893–899. Bibcode:2022Natur.603..893G. doi:10.1038/s41586-022-04521-7. PMC 9680899. PMID 35158371.
