User:Kumokumo0310/腹痛:修订间差异
→部分可能病因: // Edit via Wikiplus |
→References: // Edit via Wikiplus |
||
| 第392行: | 第392行: | ||
Abdominal pain is the reason about 3% of adults see their family physician.<ref name=Vin2014/> Rates of [[急诊室|emergency department]] (ED) visits in the United States for abdominal pain increased 18% from 2006 through to 2011. This was the largest increase out of 20 common conditions seen in the ED. The rate of ED use for nausea and vomiting also increased 18%.<ref>{{cite web | vauthors = Skiner HG, Blanchard J, Elixhauser A | title = Trends in Emergency Department Visits, 2006-2011 | work = HCUP Statistical Brief #179 | publisher = Agency for Healthcare Research and Quality | location = Rockville, MD | date = September 2014 | url = https://www.hcup-us.ahrq.gov/reports/statbriefs/sb179-Emergency-Department-Trends.jsp}}</ref> |
Abdominal pain is the reason about 3% of adults see their family physician.<ref name=Vin2014/> Rates of [[急诊室|emergency department]] (ED) visits in the United States for abdominal pain increased 18% from 2006 through to 2011. This was the largest increase out of 20 common conditions seen in the ED. The rate of ED use for nausea and vomiting also increased 18%.<ref>{{cite web | vauthors = Skiner HG, Blanchard J, Elixhauser A | title = Trends in Emergency Department Visits, 2006-2011 | work = HCUP Statistical Brief #179 | publisher = Agency for Healthcare Research and Quality | location = Rockville, MD | date = September 2014 | url = https://www.hcup-us.ahrq.gov/reports/statbriefs/sb179-Emergency-Department-Trends.jsp}}</ref> |
||
== |
== 參考文獻 == |
||
{{reflist}} |
{{reflist|2}} |
||
== External links == |
== External links == |
||
2022年5月18日 (三) 09:44的版本
| 腹痛 | |
|---|---|
| 又称 | 肚子痛 |
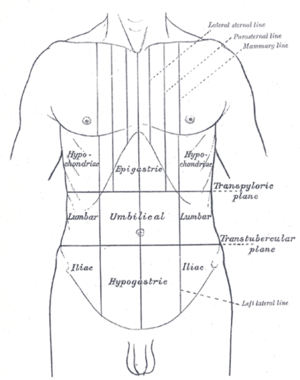 | |
| 腹痛的位置可根據其影響的器官而定。 | |
| 病因 | 嚴重病因:闌尾炎、, 胃潰瘍、胃穿孔、胰腺炎、憩室炎破裂、卵巢扭轉、腸扭轉、主動脈瘤破裂、肝臟或脾臟破裂、缺血性腸炎、缺血性心臟病[1] 常見病因:腸胃炎、大腸激躁症[2] |
| 分类和外部资源 | |
| 醫學專科 | 胃肠学、普通外科 |
腹痛(Abdominal pain)是指腹部疼痛的症狀,其背後可能的原因可能有嚴重與非嚴重的成因。常見的腹痛原因包含腸胃炎或大腸激躁症[2]。約15%的腹痛原因可能是由更嚴重的病因引起,諸如闌尾炎、腹主動脈瘤破裂、憩室炎,或是異位妊娠[2]。其中約三分之一的患者腹痛的成因不明[2]。
由於多種疾病皆可能造成不同形式的腹痛,因此對患者進行系統性地檢查及進行鑑別診斷仍然相當重要[3]。
鑑別診斷
最常見的腹痛成因為腸胃炎(13%)、大腸激躁症(8%)、泌尿道問題(5%)、胃炎(5%),或便祕(5%)等等[4]。30%的案例原因不明[5]。約10%的病人則是緣自於較嚴重的疾病,諸如膽道(膽結石或膽道收縮障礙)、胰臟(4%)相關問題、憩室炎(3%)、闌尾炎(2%),或癌症(1%)[2]。在年長病患中較常見的病因包含缺血性腸炎[6]、腸系膜缺血、腹主動脈瘤,或其他病因[7]。
腹部急症
腹部急症的定義是指在短時間內發生劇烈而持續的疼痛,且可能必須進行緊急外科手術治療。相關症狀可能會伴隨惡心、嘔吐、腹脹、發燒,或休克的症狀。急性闌尾炎最常見的腹部急症之一[8]。
部分可能病因
By system
A more extensive list includes the following:[來源請求]
- Gastrointestinal
- GI tract
- Inflammatory: gastroenteritis, appendicitis, gastritis, esophagitis, diverticulitis, Crohn's disease, ulcerative colitis, microscopic colitis
- Obstruction: hernia, intussusception, volvulus, post-surgical adhesions, tumors, severe constipation, hemorrhoids
- Vascular: embolism, thrombosis, hemorrhage, sickle cell disease, abdominal angina, blood vessel compression (such as celiac artery compression syndrome), superior mesenteric artery syndrome, postural orthostatic tachycardia syndrome
- Digestive: peptic ulcer, lactose intolerance, celiac disease, food allergies
- Glands
- Bile system
- Inflammatory: cholecystitis, cholangitis
- Obstruction: cholelithiasis, tumours
- Liver
- Inflammatory: hepatitis, liver abscess
- Pancreatic
- Inflammatory: pancreatitis
- Bile system
- GI tract
- Renal and urological
- Inflammation: pyelonephritis, bladder infection, indigestion
- Obstruction: kidney stones, urolithiasis, urinary retention, tumours
- Vascular: left renal vein entrapment
- Gynaecological or obstetric
- Inflammatory: pelvic inflammatory disease
- Mechanical: ovarian torsion
- Endocrinological: menstruation, Mittelschmerz
- Tumors: endometriosis, fibroids, ovarian cyst, ovarian cancer
- Pregnancy: ruptured ectopic pregnancy, threatened abortion
- Abdominal wall
- muscle strain or trauma
- muscular infection
- neurogenic pain: herpes zoster, radiculitis in Lyme disease, abdominal cutaneous nerve entrapment syndrome (ACNES), tabes dorsalis
- Referred pain
- from the thorax: pneumonia, pulmonary embolism, ischemic heart disease, pericarditis
- from the spine: radiculitis
- from the genitals: testicular torsion
- Metabolic disturbance
- uremia, diabetic ketoacidosis, porphyria, C1-esterase inhibitor deficiency, adrenal insufficiency, lead poisoning, black widow spider bite, narcotic withdrawal
- Blood vessels
- Immune system
- Idiopathic
- irritable bowel syndrome (IBS)(affecting up to 20% of the population, IBS is the most common cause of recurrent and intermittent abdominal pain)
If not these it may be simpler cases like motion sickness or diarrhea. The worst case food poisoning
By location
The location of abdominal pain can provide information about what may be causing the pain. The abdomen can be divided into four regions called quadrants. Locations and associated conditions include:[9][10]
- Diffuse
- Epigastric
- Heart: myocardial infarction, pericarditis
- Stomach: gastritis, stomach ulcer, stomach cancer
- Pancreas: pancreatitis, pancreatic cancer
- Intestinal: duodenal ulcer, diverticulitis, appendicitis
- Right upper quadrant
- Liver: hepatomegaly, fatty liver, hepatitis, liver cancer, abscess
- Gallbladder and biliary tract: inflammation, gallstones, worm infection, cholangitis
- Colon: bowel obstruction, functional disorders, gas accumulation, spasm, inflammation, colon cancer
- Other: pneumonia, Fitz-Hugh-Curtis syndrome
- Left upper quadrant
- Splenomegaly
- Colon: bowel obstruction, functional disorders, gas accumulation, spasm, inflammation, colon cancer
- Peri-umbilical (the area around the umbilicus, aka the belly button)
- Appendicitis
- Pancreatitis
- Inferior myocardial infarction
- Peptic ulcer
- Diabetic ketoacidosis
- Vascular: aortic dissection, aortic rupture
- Bowel: mesenteric ischemia, Celiac disease, inflammation, intestinal spasm, functional disorders, small bowel obstruction
- Lower abdominal pain
- Right lower quadrant
- Colon: intussusception, bowel obstruction, appendicitis (McBurney's point)
- Renal: kidney stone (nephrolithiasis), pyelonephritis
- Pelvic: cystitis, bladder stone, bladder cancer, pelvic inflammatory disease, pelvic pain syndrome
- Gynecologic: endometriosis, intrauterine pregnancy, ectopic pregnancy, ovarian cyst, ovarian torsion, fibroid (leiomyoma), abscess, ovarian cancer, endometrial cancer
- Left lower quadrant
- Bowel: diverticulitis, sigmoid colon volvulus, bowel obstruction, gas accumulation, Toxic megacolon
- Right low back pain
- Liver: hepatomegaly
- Kidney: kidney stone (nephrolithiasis), complicated urinary tract infection
- Left low back pain
- Spleen
- Kidney: kidney stone (nephrolithiasis), complicated urinary tract infection
- Low back pain
- kidney pain (kidney stone, kidney cancer, hydronephrosis)
- Ureteral stone pain
Pathophysiology
| Region | Blood supply[11] | Innervation[12] | Structures[11] |
|---|---|---|---|
| Foregut | Celiac artery | T5 - T9 | Pharynx
Proximal duodenum |
| Midgut | Superior mesenteric artery | T10 - T12 | Distal duodenum
Proximal transverse colon |
| Hindgut | Inferior mesenteric artery | L1 - L3 | Distal transverse colon
Superior anal canal |
Abdominal pain can be referred to as visceral pain or peritoneal pain. The contents of the abdomen can be divided into the foregut, midgut, and hindgut.[11] The foregut contains the pharynx, lower respiratory tract, portions of the esophagus, stomach, portions of the duodenum (proximal), liver, biliary tract (including the gallbladder and bile ducts), and the pancreas.[11] The midgut contains portions of the duodenum (distal), cecum, appendix, ascending colon, and first half of the transverse colon.[11] The hindgut contains the distal half of the transverse colon, descending colon, sigmoid colon, rectum, and superior anal canal.[11]
Each subsection of the gut has an associated visceral afferent nerve that transmits sensory information from the viscera to the spinal cord, traveling with the autonomic sympathetic nerves.[13] The visceral sensory information from the gut traveling to the spinal cord, termed the visceral afferent, is non-specific and overlaps with the somatic afferent nerves, which are very specific.[14] Therefore, visceral afferent information traveling to the spinal cord can present in the distribution of the somatic afferent nerve; this is why appendicitis initially presents with T10 periumbilical pain when it first begins and becomes T12 pain as the abdominal wall peritoneum (which is rich with somatic afferent nerves) is involved.[14]
Diagnosis
A thorough patient history and physical examination is used to better understand the underlying cause of abdominal pain.
The process of gathering a history may include:[15]
- Identifying more information about the chief complaint by eliciting a history of present illness; i.e. a narrative of the current symptoms such as the onset, location, duration, character, aggravating or relieving factors, and temporal nature of the pain. Identifying other possible factors may aid in the diagnosis of the underlying cause of abdominal pain, such as recent travel, recent contact with other ill individuals, and for females, a thorough gynecologic history.
- Learning about the patient's past medical history, focusing on any prior issues or surgical procedures.
- Clarifying the patient's current medication regimen, including prescriptions, over-the-counter medications, and supplements.
- Confirming the patient's drug and food allergies.
- Discussing with the patient any family history of disease processes, focusing on conditions that might resemble the patient's current presentation.
- Discussing with the patient any health-related behaviors (e.g. tobacco use, alcohol consumption, drug use, and sexual activity) that might make certain diagnoses more likely.
- Reviewing the presence of non-abdominal symptoms (e.g., fever, chills, chest pain, shortness of breath, vaginal bleeding) that can further clarify the diagnostic picture.
- Using Carnett's sign to differentiate between visceral pain and pain originating in the muscles of the abdominal wall.[16]
After gathering a thorough history, one should perform a physical exam in order to identify important physical signs that might clarify the diagnosis, including a cardiovascular exam, lung exam, thorough abdominal exam, and for females, a genitourinary exam.[15]
Additional investigations that can aid diagnosis include:[17]
- Blood tests including complete blood count, basic metabolic panel, electrolytes, liver function tests, amylase, lipase, troponin I, and for females, a serum pregnancy test.
- Urinalysis
- Imaging including chest and abdominal X-rays
- Electrocardiogram
If diagnosis remains unclear after history, examination, and basic investigations as above, then more advanced investigations may reveal a diagnosis. Such tests include:[17]
- Computed tomography of the abdomen/pelvis
- Abdominal or pelvic ultrasound
- Endoscopy and/or colonoscopy
Management
The management of abdominal pain depends on many factors, including the etiology of the pain. In the emergency department, a person presenting with abdominal pain may initially require IV fluids due to decreased intake secondary to abdominal pain and possible emesis or vomiting.[18] Treatment for abdominal pain includes analgesia, such as non-opioid (ketorolac) and opioid medications (morphine, fentanyl).[18] Choice of analgesia is dependent on the cause of the pain, as ketorolac can worsen some intra-abdominal processes.[18] Patients presenting to the emergency department with abdominal pain may receive a "GI cocktail" that includes an antacid (examples include omeprazole, ranitidine, magnesium hydroxide, and calcium chloride) and lidocaine.[18] After addressing pain, there may be a role for antimicrobial treatment in some cases of abdominal pain.[18] Butylscopolamine (Buscopan) is used to treat cramping abdominal pain with some success.[19] Surgical management for causes of abdominal pain includes but is not limited to cholecystectomy, appendectomy, and exploratory laparotomy.[來源請求]
Emergencies
Below is a brief overview of abdominal pain emergencies.
| Condition | Presentation | Diagnosis | Management |
|---|---|---|---|
| Appendicitis[20] | Abdominal pain, nausea, vomiting, fever
Periumbilical pain, migrates to RLQ |
Clinical (history & physical exam)
Abdominal CT |
Patient made NPO (nothing by mouth)
IV fluids as needed General surgery consultation, possible appendectomy Antibiotics Pain control |
| Cholecystitis[20] | Abdominal pain (RUQ, radiates epigastric), nausea, vomiting, fever, Murphy's sign | Clinical (history & physical exam)
Imaging (RUQ ultrasound) Labs (leukocytosis, transamintis, hyperbilirubinemia) |
Patient made NPO (nothing by mouth)
IV fluids as needed General surgery consultation, possible cholecystectomy Antibiotics Pain, nausea control |
| Acute pancreatitis[20] | Abdominal pain (sharp epigastric, shooting to back), nausea, vomiting | Clinical (history & physical exam)
Labs (elevated lipase) Imaging (abdominal CT, ultrasound) |
Patient made NPO (nothing by mouth)
IV fluids as needed Pain, nausea control Possibly consultation of general surgery or interventional radiology |
| Bowel obstruction[20] | Abdominal pain (diffuse, crampy), bilious emesis, constipation | Clinical (history & physical exam)
Imaging (abdominal X-ray, abdominal CT) |
Patient made NPO (nothing by mouth)
IV fluids as needed Nasogastric tube placement General surgery consultation Pain control |
| Upper GI bleed[20] | Abdominal pain (epigastric), hematochezia, melena, hematemesis, hypovolemia | Clinical (history & physical exam, including digital rectal exam)
Labs (complete blood count, coagulation profile, transaminases, stool guaiac) |
Aggressive IV fluid resuscitation
Blood transfusion as needed Medications: proton pump inhibitor, octreotide Stable patient: observation Unstable patient: consultation (general surgery, gastroenterology, interventional radiology) |
| Lower GI Bleed[20] | Abdominal pain, hematochezia, melena, hypovolemia | Clinical (history & physical exam, including digital rectal exam)
Labs (complete blood count, coagulation profile, transaminases, stool guaiac) |
Aggressive IV fluid resuscitation
Blood transfusion as needed Medications: proton pump inhibitor Stable patient: observation Unstable patient: consultation (general surgery, gastroenterology, interventional radiology) |
| Perforated Viscous[20] | Abdominal pain (sudden onset of localized pain), abdominal distension, rigid abdomen | Clinical (history & physical exam)
Imaging (abdominal X-ray or CT showing free air) Labs (complete blood count) |
Aggressive IV fluid resuscitation
General surgery consultation Antibiotics |
| Volvulus[20] | Sigmoid colon volvulus: Abdominal pain (>2 days, distention, constipation)
Cecal volvulus: Abdominal pain (acute onset), nausea, vomiting |
Clinical (history & physical exam)
Imaging (abdominal X-ray or CT) |
Sigmoid: Gastroenterology consultation (flexibile sigmoidoscopy)
Cecal: General surgery consultation (right hemicolectomy) |
| Ectopic pregnancy[20] | Abdominal and pelvic pain, bleeding
If ruptured ectopic pregnancy, the patient may present with peritoneal irritation and hypovolemic shock |
Clinical (history & physical exam)
Labs: complete blood count, urine pregnancy test followed with quantitative blood beta-hCG Imaging: transvaginal ultrasound |
If patient is unstable: IV fluid resuscitation, urgent obstetrics and gynecology consultation
If patient is stable: continue diagnostic workup, establish OBGYN follow-up |
| Abdominal aortic aneurysm[20] | Abdominal pain, flank pain, back pain, hypotension, pulsatile abdominal mass | Clinical (history & physical exam)
Imaging: Ultrasound, CT angiography, MRA/magnetic resonance angiography |
If patient is unstable: IV fluid resuscitation, urgent surgical consultation
If patient is stable: admit for observation |
| Aortic dissection[20] | Abdominal pain (sudden onset of epigastric or back pain), hypertension, new aortic murmur | Clinical (history & physical exam)
Imaging: Chest X-Ray (showing widened mediastinum), CT angiography, MRA, transthoracic echocardiogram/TTE, transesophageal echocardiogram/TEE |
IV fluid resuscitation
Blood transfusion as needed (obtain type and cross) Medications: reduce blood pressure (sodium nitroprusside plus beta blocker or calcium channel blocker) Surgery consultation |
| Liver injury[20] | After trauma (blunt or penetrating), abdominal pain (RUQ), right rib pain, right flank pain, right shoulder pain | Clinical (history & physical exam)
Imaging: FAST examination, CT of abdomen and pelvis |
Resuscitation (Advanced Trauma Life Support) with IV fluids (crystalloid) and blood transfusion
If patient is unstable: general or trauma surgery consultation with subsequent exploratory laparotomy |
| Splenic injury[20] | After trauma (blunt or penetrating), abdominal pain (LUQ), left rib pain, left flank pain | Clinical (history & physical exam)
Imaging: FAST examination, CT of abdomen and pelvis |
Resuscitation (Advanced Trauma Life Support) with IV fluids (crystalloid) and blood transfusion
If patient is unstable: general or trauma surgery consultation with subsequent exploratory laparotomy and possible splenectomy If patient is stable: medical management, consultation of interventional radiology for possible arterial embolization |
Epidemiology
Abdominal pain is the reason about 3% of adults see their family physician.[2] Rates of emergency department (ED) visits in the United States for abdominal pain increased 18% from 2006 through to 2011. This was the largest increase out of 20 common conditions seen in the ED. The rate of ED use for nausea and vomiting also increased 18%.[21]
參考文獻
- ^ Patterson JW, Dominique E. Acute Abdomenal. StatPearls. 14 Nov 2018. PMID 29083722.
- ^ 2.0 2.1 2.2 2.3 2.4 2.5 Viniol A, Keunecke C, Biroga T, Stadje R, Dornieden K, Bösner S, et al. Studies of the symptom abdominal pain--a systematic review and meta-analysis. Family Practice. October 2014, 31 (5): 517–29. PMID 24987023. doi:10.1093/fampra/cmu036
 .
.
- ^ differential diagnosis. Merriam-Webster (Medical dictionary). [30 December 2014].
- ^ 引用错误:没有为名为
Vin20142的参考文献提供内容 - ^ 引用错误:没有为名为
Vin20143的参考文献提供内容 - ^ Hung, Alex; Calderbank, Tom; Samaan, Mark A.; Plumb, Andrew A.; Webster, George. Ischaemic colitis: practical challenges and evidence-based recommendations for management. Frontline Gastroenterology. 1 January 2021, 12 (1): 44–52. ISSN 2041-4137. doi:10.1136/flgastro-2019-101204 (英语).
- ^ Spangler R, Van Pham T, Khoujah D, Martinez JP. Abdominal emergencies in the geriatric patient. International Journal of Emergency Medicine. 2014, 7: 43. PMC 4306086
 . PMID 25635203. doi:10.1186/s12245-014-0043-2.
. PMID 25635203. doi:10.1186/s12245-014-0043-2.
- ^ Appendicitis. The Lecturio Medical Concept Library. [1 July 2021].
- ^ Masters P. IM Essentials. American College of Physicians. 2015. ISBN 9781938921094.
- ^ LeBlond RF. Diagnostics. US: McGraw-Hill Companies, Inc. 2004. ISBN 978-0-07-140923-0.
- ^ 11.0 11.1 11.2 11.3 11.4 11.5 Moore KL. 11. The Developing Human Tenth Edition. Philadelphia, PA: Elsevier, Inc. 2016: 209–240. ISBN 978-0-323-31338-4.
- ^ Hansen JT. 4: Abdomen. Netter's Clinical Anatomy, 4e. Philadelphia, PA: Elsevier. 2019: 157–231. ISBN 978-0-323-53188-7.
- ^ Drake RL, Vogl AW, Mitchell AW. 4: Abdomen. Gray's Anatomy For Students Third. Churchill Livingstone Elsevier. 2015: 253–420. ISBN 978-0-7020-5131-9.
- ^ 14.0 14.1 Neumayer L, Dangleben DA, Fraser S, Gefen J, Maa J, Mann BD. 11: Abdominal Wall, Including Hernia. Essentials of General Surgery, 5e. Baltimore, MD: Wolters Kluwer Health. 2013.
- ^ 15.0 15.1 Bickley L. Bates' Guide to Physical Examination & History Taking. Philadelphia, Pennsylvania: Lippincott Williams & Wilkins. 2016. ISBN 9781469893419.
- ^ ANP-BC, Karen M. Myrick, DNP, APRN, FNP-BC; ANP-BC, Laima Karosas, PhD, APRN, FNP-BC. Advanced Health Assessment and Differential Diagnosis: Essentials for Clinical Practice. Springer Publishing Company. 2019-12-06: 250. ISBN 978-0-8261-6255-7 (英语).
- ^ 17.0 17.1 Cartwright SL, Knudson MP. Evaluation of acute abdominal pain in adults. American Family Physician. April 2008, 77 (7): 971–8. PMID 18441863.
- ^ 18.0 18.1 18.2 18.3 18.4 Mahadevan SV. Essentials of Family Medicine 6e. : 149.
- ^ Tytgat GN. Hyoscine butylbromide: a review of its use in the treatment of abdominal cramping and pain. Drugs. 2007, 67 (9): 1343–57. PMID 17547475. S2CID 46971321. doi:10.2165/00003495-200767090-00007.
- ^ 20.00 20.01 20.02 20.03 20.04 20.05 20.06 20.07 20.08 20.09 20.10 20.11 20.12 Sherman SC, Cico SJ, Nordquist E, Ross C, Wang E. Atlas of Clinical Emergency Medicine. Wolters Kluwer. 2016. ISBN 978-1-4511-8882-0.
- ^ Skiner HG, Blanchard J, Elixhauser A. Trends in Emergency Department Visits, 2006-2011. HCUP Statistical Brief #179. Rockville, MD: Agency for Healthcare Research and Quality. September 2014.
